From Toddlers to Teens…We are actively screening children and adolescents (ages 1-17) with spinal cord injuries for enrollment in:
Please Contact Us to learn more. Activity-based Therapy – Locomotor Training
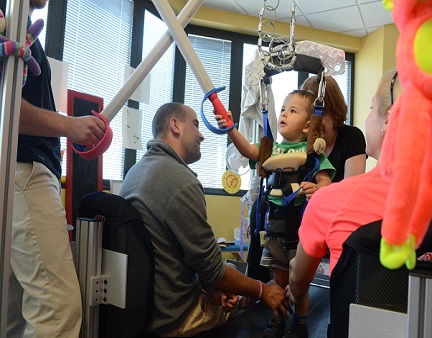
Just like a child who practices soccer every day of the week to hone their skills, children who have suffered a severe insult to their nervous systems also require intense training to see results. Locomotor training is an intense, activity-based therapy designed to activate the neuromuscular system below the level of a spinal cord injury or neurological impairment and restore function in weak or paralyzed muscles. During locomotor training, the child is suspended in a harness over a treadmill and facilitated by therapists to step and stand with the timing and movements similar to those used prior to injury or that are age-appropriate, i.e. “train like you walk”. Specific sensory cues are used along with a body weight support system on a treadmill to activate age-expected movement patterns for standing, walking and trunk control. These specific cues provide a “picture” of walking or standing to the nervous system and promote “turning on” the system, thought to be inactive or paralyzed after injury. Newly developed motor skills are then applied to the child’s everyday activities (off the treadmill). This combined with increased specific activities at home and in the community allows for the emergence of motor and other functions not seen since injury. In the case of some children injured prior to the development of sitting, standing, or walking, these functions may never have been seen before. This approach is in stark contrast to traditional approaches, such as the primary use of wheelchairs, standing frames, braces, and assistive devices, which focus on compensation for injury-induced weakness and paralysis. Comprehensive Assessment
Your child’s progress will be assessed by on-going re-evaluations performed after every 20 sessions of locomotor training. Upon completion of an episode of locomotor training (60 sessions or greater), a discharge evaluation will be completed by the physician and the physical therapist. Annual Follow-up Evaluations
Scheduled CommunicationsBecause activity-based therapies are most successful when the principles are incorporated throughout the day, what happens at home, school and in community settings is very important to your child’s continued recovery. Therefore, we value ongoing communication with families to address issues, concerns, and needs related to recovery as they arise. While your child is enrolled in the Locomotor Training program, a team member will meet with you weekly to discuss your child’s progress and address any concerns. Families may contact us at any time with questions and concerns in regard to their child’s recovery, and we will pursue answers and provide evidence-based information as appropriate. At time of discharge, we will meet with the family to discuss the outcomes of our discharge evaluation, finalize a plan for continuation of principle-based activities in the home and community specific to your child’s progress and needs, and plan for your next visit (e.g. schedule follow-up date). After discharge from an episode of out-patient therapy, we will schedule and conduct quarterly phone communications to gather information regarding your child’s continued progress with recovery and any factors affecting progress. This information assists us in identifying steps forward and challenges that your child and you may face so that they may be productively addressed. |
The Kosair for Kids Center for Recovery-Based Therapies: Pediatric NeuroRecovery Research |


 An activity-based therapy is a physical rehabilitation therapy that’s purpose is to “activate” or “turn on” the nerves and muscles affected by a neurological impairment. The activity refers to the specific type and amount of practice and input that is necessary to elicit an improvement in a motor skill. The type of activity is task-specific such that we “train like you walk” and “train like you stand”. The amount of activity refers to the intensity of practice and input necessary for the child’s abilities to improve. Therapy sessions occur daily (5 times/week) for 1.5 hours/day for a minimum of 60 sessions. Additional sessions may be indicated based on your child’s progress and need.
An activity-based therapy is a physical rehabilitation therapy that’s purpose is to “activate” or “turn on” the nerves and muscles affected by a neurological impairment. The activity refers to the specific type and amount of practice and input that is necessary to elicit an improvement in a motor skill. The type of activity is task-specific such that we “train like you walk” and “train like you stand”. The amount of activity refers to the intensity of practice and input necessary for the child’s abilities to improve. Therapy sessions occur daily (5 times/week) for 1.5 hours/day for a minimum of 60 sessions. Additional sessions may be indicated based on your child’s progress and need. Some of these assessments your child may be familiar with, others may be completely new. We strive to make the assessments “child-friendly” and use age-appropriate behavior techniques to engage the child and maximize participation.
Some of these assessments your child may be familiar with, others may be completely new. We strive to make the assessments “child-friendly” and use age-appropriate behavior techniques to engage the child and maximize participation. Our rehabilitation and medical team conducts comprehensive clinical evaluations viewing your child’s health and well-being through a lens of “recovery” and development. Annual evaluations are important to assess the impact of growth and development on your child’s long-term recovery and quality of life. Our team meets with parents to discuss child progress and state of recovery and develop the next steps for therapy and home. We expect that after completing an initial episode of locomotor training (minimum 60 sessions), that a child will return yearly for “booster” sessions to address new potential, developmental changes, physical growth, and differences in environmental stresses. We anticipate with certain life transitions, such as moving from elementary to middle school, the child may face new neuromotor demands and require additional intervention to foster continued recovery. A child’s annual evaluation is scheduled six months to a year in advance.
Our rehabilitation and medical team conducts comprehensive clinical evaluations viewing your child’s health and well-being through a lens of “recovery” and development. Annual evaluations are important to assess the impact of growth and development on your child’s long-term recovery and quality of life. Our team meets with parents to discuss child progress and state of recovery and develop the next steps for therapy and home. We expect that after completing an initial episode of locomotor training (minimum 60 sessions), that a child will return yearly for “booster” sessions to address new potential, developmental changes, physical growth, and differences in environmental stresses. We anticipate with certain life transitions, such as moving from elementary to middle school, the child may face new neuromotor demands and require additional intervention to foster continued recovery. A child’s annual evaluation is scheduled six months to a year in advance.